
By now you know that Bloodworks is more than just a blood center.
Bloodworks’ Immunohematology Reference Laboratory (IRL) and Genomics Testing Laboratory work around the clock every day of the year to provide complex immunohematological and genomic testing services for more than 90 institutions from Alaska to Oregon – over 10,000 tests each year!
Immunohematology as a field encompasses hematology, immunology, and genetics. Bloodworks’ labs identify antibodies and antigens on red blood cells to determine the best match for patients.
“When a patient has a reaction to a blood transfusion, we have to figure out why,” said Lay See Er, IRL Manager. “And of course, find the best possible blood that’s safe for transfusion.”
As a blood donor, you understand that your blood type is one of eight main blood types, as determined by the ABO and Rh blood group systems; these are the major blood group systems, but they’re actually just two of 45 different blood group systems! Blood types are genetic, meaning you inherit your blood type from your parents.
Blood groups are essentially the presence or absence of certain antigens, proteins that are part of the body’s immune response, on red blood cells.
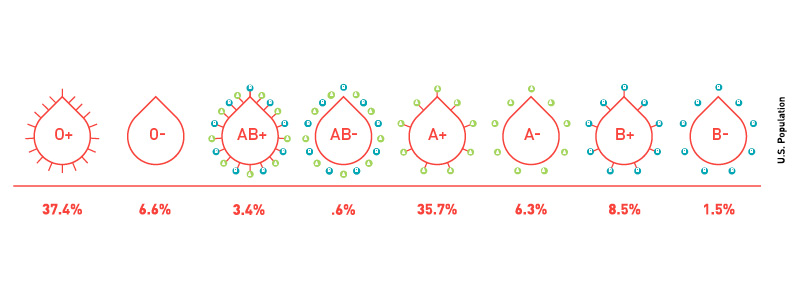
For most patients, matching ABO and Rh is sufficient.
However, red cells have over 360 different variations of other proteins beyond ABO and Rh.
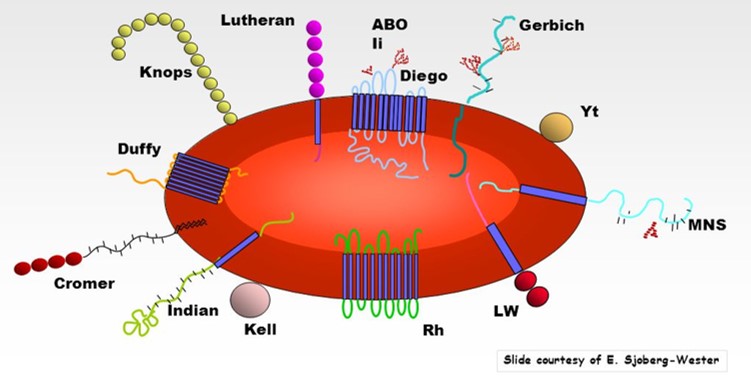
Patients who receive frequent transfusions may develop antibodies against antigens from these other blood groups.
“For those who require regular blood transfusions for ongoing disease management, such as sickle cell anemia and thalassemia, each transfusion increases the risk that they can develop antibodies, and their body could reject future transfusions if not matched as closely to their own antigens as possible,” said Lay See.
When a patient does have a transfusion reaction, IRL does the complex testing to understand why.
“Regular patient draws prior transfusion allows IRL to test for new red cell antibodies and find a matching donor so that reactions do not occur,” explained Dr. Theresa Nester, Co-Chief Medical Officer.
Bloodworks also works with labs around the country — and world — to source blood for local patients if suitable units cannot be found within our donor pool and to match Bloodworks donors with patients elsewhere.
An example where this may be needed is with a blood group protein that is found on most red blood cells (high prevalence), making blood that doesn’t have this antigen uncommon or even rare.
IRL also maintains an inventory of both fresh and frozen antigen-negative red cell units to support patients with single or multiple antibodies, as well as those with antibodies against high prevalence antigens.
“Rare red cells can be kept in a frozen state for up to 10 years,” said Dr. Nester. “The IRL has special equipment and procedures required to thaw and prepare that unit for transfusion.”
Zainab is a little girl in Florida with some of the rarest blood in the world: she is missing a common red cell antigen that most people have on their red blood cells called “Indian B” (Inb). Zainab can only receive transfusions from people who are also negative for Inb or her body will reject the blood.
Finding compatible donors to help Zainab combat neuroblastoma, a form of nerve cell cancer, was a worldwide effort.
People of Indian, Iranian, or Pakistani descent are most likely to be Inb negative, and even out of these populations, fewer than 4% are.
After OneBlood put out a plea for South Asian donors, more than 25,000 people who met the criteria to be a potential match for Zainab responded.
At Bloodworks, IRL worked closely with our Donor Care Team to recruit and then screen over 100 potential donors. IRL is a member of the American Rare Blood Donor Program (ARDP), a national organization whose mission is to ensure that rare blood, like Zainab’s, is available for the patients who need it.
These efforts found two donors in the United States, two in the United Kingdom, and one in Australia and helped Zainab get through two bone marrow transplants and radiation and immunotherapy treatments.
As Zainab’s story shows, “in some unique cases, to find a matching blood type for a patient in need, the best outcomes are nearly always found from a donor within the same ethnic group to which the patient belongs,” Lay See said.
“As the population of the United States continues to become more racially and ethnically diverse, IRL continues to focus on recruitment and retention of donors from underrepresented communities to maintain a safe and adequate blood supply, improving patient care in the Pacific Northwest.”
With such a complex field, it’s no surprise that IRL scientists need extensive training in a range of serological techniques, the tests that detect antibodies within blood. It takes approximately two years to learn the full range of lab procedures.
All IRL testing scientists are certified through the American Society for Clinical Pathology [MLT(ASCP)], at the very minimum. MLT (ASCP) credentialing covers Blood Banking, Urinalysis and Other Body Fluids, Chemistry, Hematology, Immunology, Microbiology, and Laboratory Operations.
Many IRL staff also have Specialist in Blood Banking Technology, SBB(ASCP) Certification, which covers all aspects of blood banking, from routine testing to highly specialized procedures.
It takes dedication to become an IRL scientist, but it’s all about saving lives. And this work isn’t possible without blood donors like you.
Tell Us What You Think!