In addition to the extensive measures taken at Bloodworks to ensure an adequate and safe blood supply, Bloodworks scientists dedicate a great deal of effort to understanding the functions of the cells and proteins of the blood and their roles in health and disease.
One cell that people usually don’t think about as being a blood cell is the endothelial cell, the cells that line blood vessels. This is because we examine blood by drawing it out of the body and looking at it with microscopes or testing it biochemically.
However, unlike platelets, red cells, or white cells, endothelial cells do not circulate and can’t be studied in this way. Yet, endothelial cells are always in contact with the rest of the blood, serving as a kind of continuous tiling, lining the insides of blood vessels large and small. Even the inner surfaces of the heart chambers and the heart valves are lined with endothelial cells.
Because of their position at the interface between blood and tissues, endothelial cells are vital to the normal functions of blood, keeping it liquid and flowing, manufacturing various hormones and other substances that affect its function, and signaling to white blood cells where and when they should leave the bloodstream to combat microbial invaders.
The interactions between endothelial cells and other blood cells also have important roles in many common and rare diseases. For example, hardening of the arteries (atherosclerosis) begins and progresses because high levels of “bad” cholesterol (LDL cholesterol, usually elevated because of high consumption of animal fat) activate the endothelial cells to become sticky, capturing platelets and white cells and leading to the deposition of cholesterol in the artery wall and causing important vessels to narrow and eventually occlude (close up).
Ultimately, the long, slow progression of atherosclerosis can lead to sudden death due to a heart attack or stroke.
Another common disease for which we (the López and Chung laboratories at Bloodworks working in collaboration with Dr. Jonathan Lindner at the University of Virginia) have found a role for the endothelial/blood cell interaction is aortic stenosis. Aortic stenosis refers to narrowing of the aortic valve, a structure between the outlet of the left ventricle of the heart and the biggest artery in the body, the aorta. Progressive narrowing of the valve puts an ever-increasing load on the heart, eventually leading to heart failure. It is estimated that over 20% of Americans over age 65 have some degree of aortic stenosis.
Our studies showed that mice that lacked the enzyme ADAMTS13 had more rapid progression of aortic stenosis. ADAMTS13 cleaves the sticky blood protein von Willebrand factor to regulate hemostasis. Von Willebrand factor normally helps blood clot, but can adhere to heart valve surfaces and lead to valve narrowing.
Narrowing of the aortic valve proceeded even more rapidly if the mice were also made hypercholesterolemic (high cholesterol) with a high-fat diet.
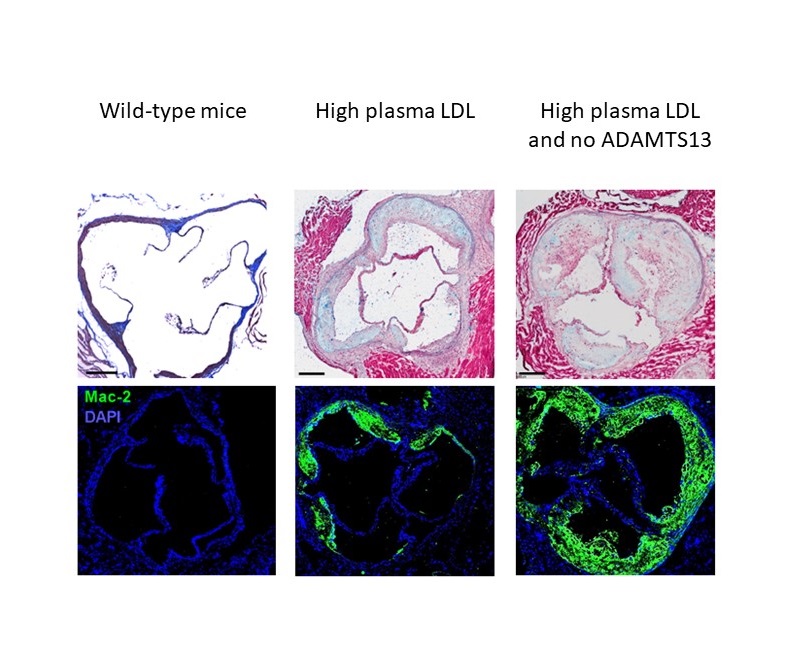
These findings provided the first evidence for factors that could be modified (e.g., the diet) to prevent aortic stenosis or slow its progression and also provided targets for pharmaceutical intervention.
This brief example highlights once again the many ways that understanding blood can lead to improvements in human health, even in conditions without an obvious blood connection.
Dr. José López is Bloodworks Research Institute’s Chief Scientific Officer.
Tell Us What You Think!