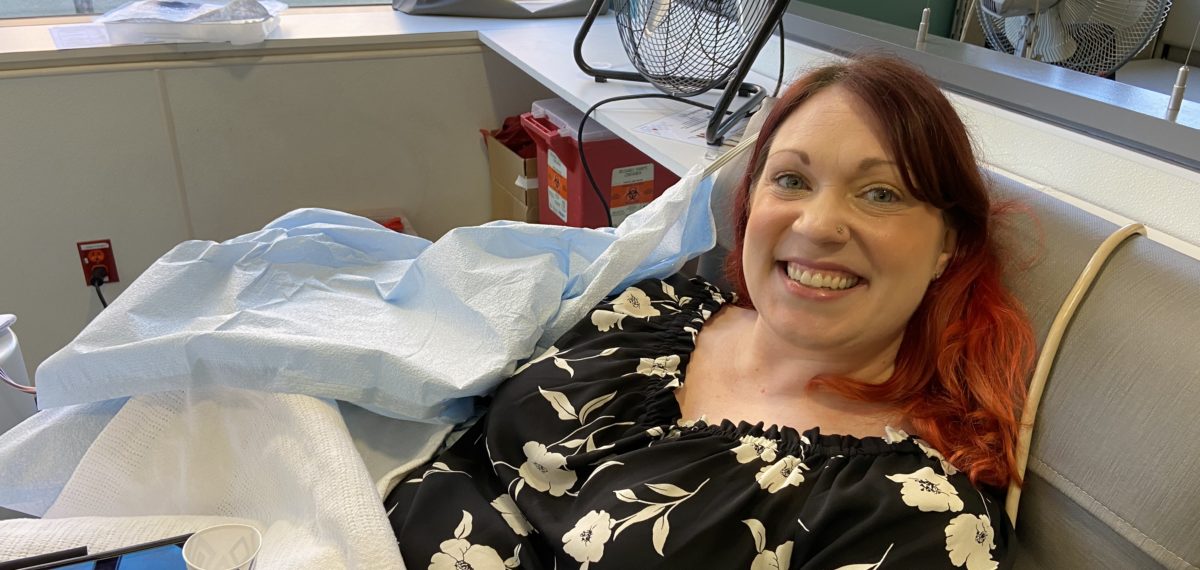
Seattle’s Elizabeth Schneider is Bloodworks Northwest’s first Convalescent Plasma donor. Convalescent Plasma is donated by those who’ve tested positive for COVID-19, have recovered and have a clean bill of health for 28 days. In a story with too few happy endings, stories like Elizabeth Schneider’s offer the world a measure of something that’s been in short supply – hope.
Listen below or read on for a full transcript.
Elizabeth Schneider is our first convalescent plasma donor. Convalescent plasma is donated by those who’ve tested positive for COVID-19, recovered & have a clean bill of health for 28 days. Stories like Elizabeth’s offer the world a measure of hope. https://t.co/fjM3UR2WNx pic.twitter.com/8ZnCncJ5kX
— Bloodworks Northwest 🩸 (@BloodworksNW) April 27, 2020
John: This edition of “Bloodworks 101” is sponsored by USI Insurance Services, harnessing the power of one advantage. Visit usi.com to learn more. “Bloodworks 101” is also sponsored by Swedish. Visit swedish.org/healthforgood.
Linmara: Oh, I had no idea. I had no idea. I had no idea how serious this was.
John: Hi, I’m John Yeager and this is “Bloodworks 101.” It’s a monthly podcast produced by Bloodworks Northwest, a Seattle-based nonprofit providing blood and blood products to almost 100 hospitals across the Pacific Northwest. Today, you’re going to meet a woman named Linmara Bluebird and one of the people who helped save her life. I’ll never forget the day I first met Linmara Bluebird. Well, that’s a name you don’t easily forget but this is not a story about a name.
It was the Pride Parade in June, 2019. Like everyone else in the parade at the Bloodworks Northwest float, when Linmara Bluebird was wearing a Bloodworks Northwest t-shirt. She was in good spirits, everybody was. It was a day of unity and happiness and I remember the sun was shining, but that’s not what struck me that day. It was the sign that Linmara Bluebird held. It read, “BWNW, Bloodworks Northwest saved my life.” She walked everywhere with it. So this is the story of why she held it.
Linmara: Well, I have learned to be more careful about my health.
John: That lesson started a year and a half ago on a cold January morning. Linmara Bluebird thought she’d just pulled a muscle.
Linmara: And I woke up that morning, it was a Friday, and I fainted. And I had a pain in my right leg. I didn’t give it too much thought. And by Monday, I noticed that my leg was bruising and was getting swollen. I swim so I felt like I couldn’t walk. I was getting kind of winded. So I went swimming all week and was very winded and I still thought, “Oh, I probably pulled a hamstring.”
John: But when she went to get it checked out, her doctor took one look at Linmara’s leg and said…
Linmara: “I have never seen a leg that looks like that.” It was blue, it was bruised, it was painful. And said, “I should take you to the emergency room but let us do some blood work.” She took some blood. This was Friday afternoon around 5:00. She was going on vacation the next week. It was a holiday weekend. So I got a phone call at 9:00 Friday night, “You need to get to the emergency room. This is looking serious.”
John: Linmara and her partner live on Bainbridge Island. They went to the closest hospital, Harrison in Bremerton.
Linmara: They admitted me. I was in there most of the night. I was in some pain, couldn’t get comfortable. They took some blood.
John: She didn’t know what to expect.
Linmara: Oh, I had no idea. I had no idea. I had no idea how serious this was.
John: But soon, she would. The diagnosis sounded scary.
Linmara: I was diagnosed with acquired hemophilia A. So acquired means not genetic, comes out of the blue, a healthy person, and all of a sudden, I have internal bleeding and my clotting factor VIII was not working. When they said you have hemophilia, I’m thinking, “Where did that come from?” But acquired hemophilia is basically like many other clotting factors, one in a million.
John: According to the Centers for Disease Control and Prevention, hemophilia is usually an inherited bleeding disorder in which the blood does not clot properly. This can lead to spontaneous bleeding as well as bleeding following injuries or surgery. Blood contains many proteins called clotting factors that can help stop bleeding. People with hemophilia have low levels of either factor VIII or factor IX. The severity of hemophilia that a person has is determined by the amount of factor in the blood. The lower the amount of the factor, the more likely it is that bleeding will occur, which can lead to serious health problems.
In rare cases like Linmara’s, a person can develop hemophilia later in life. Now, it was Saturday morning and the doctor at Harrison, Tony Roberts from Poulsbo told her over the phone that she could see her.
Linmara: But she said, “I think you should see Rebecca Kruse-Jarres in Seattle, Bloodworks Northwest.” Now, I live on Bainbridge. I have to take a ferry over to Seattle but I wanted to go to the best. If she’s the one who does research, she knows about the factors, well, that’s where I’m going to go. So I came into Seattle on Tuesday morning and saw her. She agreed I have acquired hemophilia A and said, “I know what we are going to do.” She put me on prednisone at 40 milligrams.
John: And a medication typically used on cancer patients called cyclophosphamide.
Linmara: But she said, “The two of them work well together.” And I also needed a medication called Novoseven, which is an injectable medication. It’s like an emergency medication. If I was given factor VIII because my factor VIII is not working, my body would reject it. This is an autoimmune disorder. So my body is fighting factor VIII and so they can’t give me factor VIII. So Novoseven is a factor VII that appears to your body to work. And so I needed two injections of that. And over the course of, I’d say, a month and a half, I needed to have that done four times.
John: This rare combination of life-saving drugs began to make a difference.
Linmara: So this medication, by the way, is not available anywhere, but at a blood center that has it. The hospitals don’t have it. So they had to order it from Bloodworks Northwest. This has been Friday night. So I had to go home with some two doses and put them in my refrigerator. So whenever it was needed, like when the fire department needed to give me one dose when I had another bleed, they had to call Rebecca. She had to talk to them and then they administered it because I had it in my refrigerator.
John: And this was expensive medicine.
Linmara: Each dose was $10,000. Eventually, I had to have 8 doses and I had 2 in my refrigerator that I had paid for.
John: And yes, if you were wondering, Bluebird had health insurance.
Linmara: Medicare paid everything.
John: Even with all that she went through, Linmara Bluebird still considers herself…
Linmara: …incredibly, incredibly lucky.
John: Lucky because she had insurance but also because of the world class expert in blood disorders you’re about to meet. That’s coming up next when “Bloodworks 101” continues. This edition of “Bloodworks 101” is sponsored by USI Insurance Services, harnessing the power of one advantage. Visit usi.com to learn more. “Bloodworks 101” is also sponsored by Swedish. Visit swedish.org/healthforgood.
Welcome back to “Bloodworks 101,” I’m your host, John Yeager. Dr. Rebecca Kruse-Jarres at the Washington Centre for Bleeding Disorders says something like acquired hemophilia that hit Linmara from out of the blue is usually not picked up very frequently.
Dr. Kruse-Jarres: People usually think it’s a pulled muscle, it’s an injury that seems to be maybe having some bruising and swelling over the top but nobody thinks about a bleeding disorder because these people are born normal. They don’t have a bleeding disorder to begin with and that’s not on their radar. Acquired hemophilia is a bleeding disorder that is caused by our body making an autoantibody, so an antibody against something in our body that they shouldn’t so it’s an autoimmune disease.
John: And Rebecca says it’s very, very rare.
Dr. Kruse-Jarres: It happens one in a million and sometimes, it’s associated with people who have other autoimmune conditions such as some thyroid disease, some other rheumatoid arthritis, things like that.
John: And Kruse-Jarres says it can literally come out of nowhere.
Dr. Kruse-Jarres: Because it’s not well-recognized, because these people are not born with it, so they’re not gonna come to you and say, “I have a bleeding disorder.” They come with abnormal bleeding that a lot of people are not thinking that there is something going on in the blood that’s causing it. For example, there was this patient we had in Eastern Washington that I got called on. This lady presented with swelling in her arm that turned out to be what we call compartment syndrome, meaning there is too much pressure in a compartment in the arm compressing the nerve and the artery and therefore, not supplying blood to the fingers. And at that point, you have to open up that space to release the pressure.
So this happened. Nobody was really thinking what was causing that. They did what they needed to do emergently and did what’s called a fasciotomy or a release of the space. And she was bleeding, bleeding, bleeding, and at that point still, nobody thought about why is this lady bleeding as much as she does. And they thought, “Maybe they nicked an artery and that’s what she’s bleeding from,” took her back to the operating room, could not stop the bleeding, and ultimately amputated her arm, which is something that maybe could have been prevented if we would have known that she had acquired hemophilia to begin with.
John: So what did she prescribe for Linmara Bluebird given all she’d been through?
Dr. Kruse-Jarres: For Linmara, the treatment for acquired hemophilia is twofold. One of them, we need to stop the bleeding because we didn’t want her to develop this compartment syndrome. So we needed to give her something to stop the bleeding. You can’t give regular factor VIII because we have this antibody against it. So that’s not something that’s gonna be working. So what we use is what we call a bypassing agent and that might be a factor VII or there is another factor concentrate that’s called a prothrombin complex concentrate. And there are a couple of other treatments to kind of circumvent this antibody to stop the bleeding. And the other thing you need to do is to get rid of that antibody so that this disease state really goes away.
John: Kruse-Jarres admits her center is a magnet for cases like this because she’s published in the field and she’s well known for her work with acquired hemophilia.
Dr. Kruse-Jarres: Hopefully, I will get these calls and hopefully, anybody who reads or hears this will call us. It’s a very, very complex condition to treat because this, as I said, happens in elderly people. The older we get, the more prone we are to clotting as well. So this is a bleeding disorder that comes out of nowhere in a patient that potentially is also at risk for clotting. So it really needs a lot of expertise to handle those patients.
John: What does she want people to know?
Dr. Kruse-Jarres: I want them to know that if there’s even the slightest question about having a patient like that, we can be reached 24/7. We have a consultation service to patients and to providers, to your physicians, to anybody. So they can reach us and say, “I’m experiencing these symptoms,” or, “I have a patient that has X, Y, Z, can I run this case by you,” so we can bring the expertise to them as soon as possible.
John: As of July 2018, Linmara Bluebird was in remission.
Linmara: And the remission means that your body is sustaining that without any medication. I have to remind myself that I have this disease that I will always have. I can be in remission but it’s always in the back of my mind. And now, I’ve been having blood draws every three months. It’s gone from three times a week to once a week, to once a month. And she said, “If this last blood draw is as good as they’ve been,” that I don’t even need to come in anymore.
John: The funny thing is before all this happened, Linmara Bluebird was a regular, devoted blood donor. Now because of the hemophilia, strict FDA regulations do not allow her to donate anymore ever. But she still found a way to give.
Female: Are you here to donate today?
Linmara: Yes, I am.
John: If you come by the Bloodworks Northwest central donation center on Seattle’s First Hill, you just might notice the person at the desk when you check in.
Female: And do you have an appointment?
Linmara: Yes.
Female: Okay, great.
John: So Linmara Bluebird, the lady with the sign, has two messages she’d like you to keep in mind. One of them, she mentions to make you think.
Linmara: It can happen to anyone.
John: And the other, well, remember the message that was written on the sign she held that day?
Linmara: Bloodworks Northwest saved my life.
John: The Washington Centre for Bleeding Disorders is located at 921 Terry Avenue, Seattle, Washington 98104. Dr. Kruse-Jarres says consultation is available 24 hours a day to help patients, families, and physicians assess symptoms and get effective treatment like Linmara’s case, when acute bleeding problems occur. I should also add that Linmara told me she did eventually find a way to donate blood for research purposes. Well, that’s just about it for this episode of “Bloodworks 101.” If you have an idea for an upcoming show or someone we should talk to, please let us know. We’re at bloodworksnw.org. But in the meantime, please share this episode with your friends. For “Bloodworks 101,” I’m John Yeager. See you next time.
Subscribe to Bloodworks 101 wherever you listen to your favorite podcasts and join our Podcast Insiders group on Facebook.
Tell Us What You Think!