When Kristin Kleinhofer’s leukemia returned, her mom did some research.
“And she kept telling me, because you don’t have a match, I really want you to have cord blood. It was the whole thing about a lower rate of cancer relapse. Also, the lower chance of graft versus host disease, which is usually something that just really derails people’s quality of life post-transplant.”
Car-T therapy using Kristin’s own stem cells cured her cancer; a cord blood transplant from a public cord blood bank ensured that it didn’t come back.
While the landscape of medical treatments evolves and more options become available, cord blood transplants remain a crucial — and sometimes the only — option for many patients.
Bloodworks’ public Cord Blood Donation Program facilitates lifesaving transplants and provides hope and healing to patients like Kristin.
More than 1 in 200 people will need a stem cell transplant in their lifetime to cure blood cancer, sickle cell disease, or many other conditions. Stem cells are unspecialized cells in our bloodstream that can mature to become any type of tissue or organ cell. A stem cell transplant can restore the body after intensive treatments like chemotherapy or radiation or, with blood cancers like leukemia, may actually fight the cancer itself.
You have likely heard of the need to “find a matching donor” for a patient in need of a stem cell transplant – someone whose human leukocyte antigens (HLA) closely match their own. HLA is part of the immune system: protein markers on your cells that determine what belongs in your body and what doesn’t. Without a close HLA match, a patient’s body will reject the donor’s cells.
A patient in need of a stem cell transplant may have a few options:
The type of stem cell transplant received by the patient will depend on their specific illness, available donors, their body’s response to chemotherapy and other treatments, their overall health, and many other factors.
The more options of all types of stem cell transplant available to patients, including cord blood, the better the outcome.
Cord blood transplants are used to treat over 80 diseases and disorders, such as blood cancers like leukemia and lymphoma and sickle cell disease.
Despite being an invaluable resource, most umbilical cord blood is routinely discarded as medical waste. Saving and preserving cord blood in a frozen state, called cord blood banking, provides options for patients who would otherwise not have access to a potentially life-saving transplant resource.
Umbilical cord blood donated to public cord blood banks is used for about 10% of stem cell transplants facilitated through NMDP (formerly known as National Marrow Donor Program and Be the Match), the national stem cell registry.
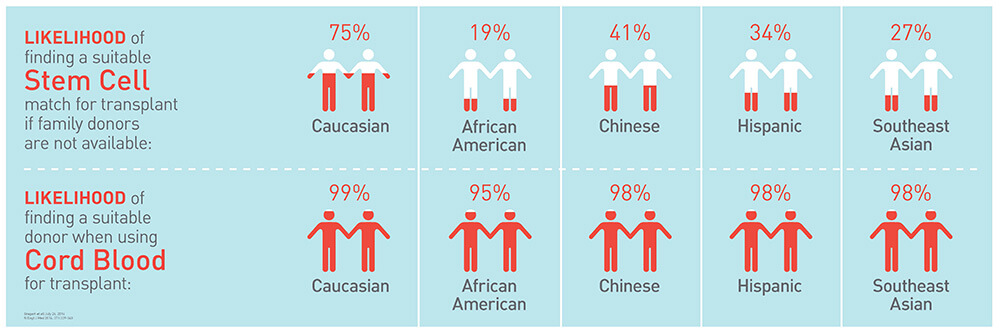
Patients from diverse racial and ethnic backgrounds have a challenging time finding a perfect match. But cord blood with a less-perfect match can be used with similar clinical outcomes, which means that racial and ethnic minorities have more opportunity for treatment.
And researchers, such as Filippo Milano, MD, PhD of Fred Hutchinson Cancer Center, are continually finding new uses for this lifesaving resource.
Public cord blood donation is an important part of Bloodworks’ lifesaving mission: we’re home to the first and only public cord blood bank in the Pacific Northwest.
The American College of Obstetricians and Gynecologists (ACOG) states, “Public umbilical cord blood banking is the recommended method of obtaining umbilical cord blood for use in transplantation, immune therapies, or other medically validated indications.”
In the case of many diseases, such as blood cancers, public banks matter because one’s own cord blood cannot be used as treatment, since it likely contains the predisposition for the condition being treated and will not be curative.
In more than 20 years, our Cord Blood Donation Program has banked over 15,500 cords for transplant and sent out 1200 units to patients in need. In 2023, we banked 273 donated cord blood units and distributed 18 for transplant.
Public cord blood donation is free and can be arranged in advance or until active labor. It does not impact the birth process or family bonding afterwards.
With public cord blood donation, like Bloodworks’ Cord Blood Donation Program, cord blood is collected and sent to a local cord blood bank, where it is evaluated and, if it meets the US FDA’s rigorous regulatory standards for banking and transplantation, stored in a controlled environment until it matches with a patient in need of a transplant.
“We work hard with our clinical partners to make sure they’re optimizing the collection to make sure it’s the best possible treatment it can be,” said Evan Delay, RN, Director of Bloodworks Bio Donation Programs.
Public cord blood banks operate under strict regulations to provide donated cord blood for any patient in need. Unlike private banks, which store cord blood for personal use, our focus remains on community health and broader accessibility.
Learn more at BloodworksNW.org/cordblood
Tell Us What You Think!