
Every two seconds, someone in the United States requires a blood transfusion. And it is in large part thanks to the pioneering research of Dr. Charles Drew, whose revolutionary work changed the landscape of blood collection and storage and, historians say, saved the lives of millions of soldiers in WWII, that today we have blood banks in our communities to help people when they need blood to live.
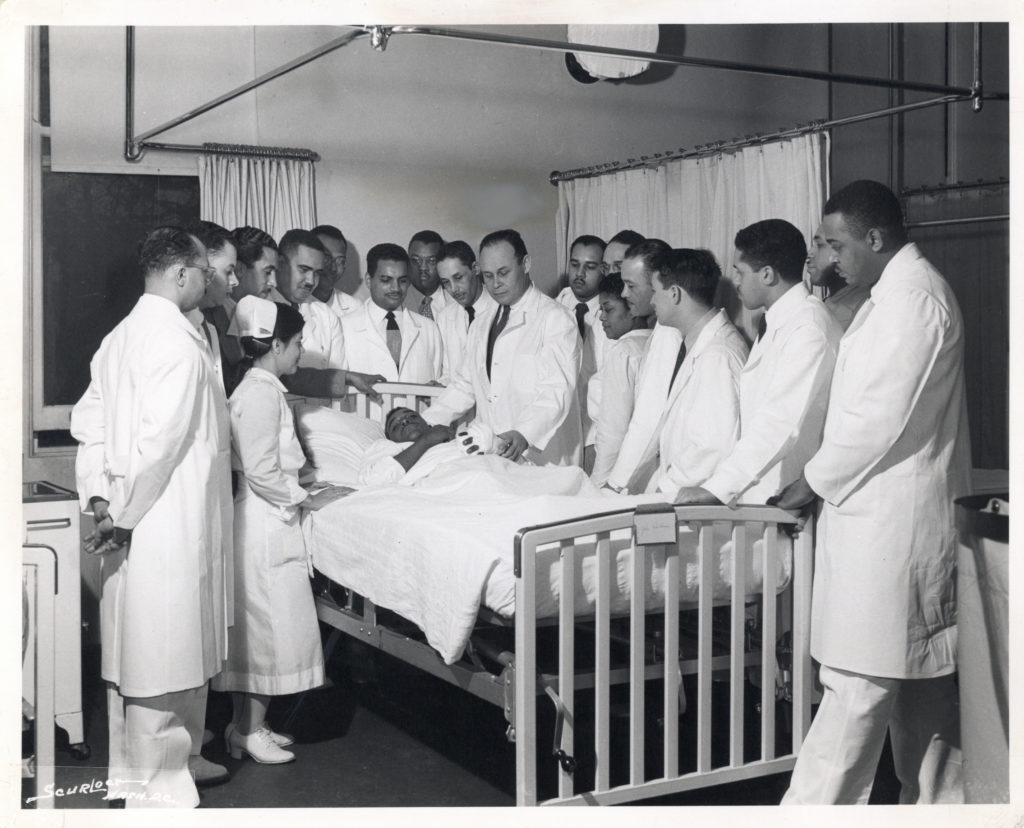
“He was a giant in our industry,” said OneBlood Chief Technical Officer Dr. Mike Pratt, who also describes Drew’s research as forming the basis for what would later become cross-matching compatibility testing, which is used in blood banks all over the world today. But it is for what Dr. Charles Drew did for blood stabilization and preservation that his work’s legacy endures today.
Drew’s doctoral dissertation, “Banked Blood: A Study in Blood Preservation,” described the novel methods he’d developed during his studies as a Rockefeller Fellow at Columbia University’s Presbyterian Hospital in New York in 1939 to separate plasma from the other blood components and lyophilize – or freeze-dry – it for long-term storage. This revolutionary discovery created a product that could be stored for two months instead of the one week that whole blood remained viable at the time, and would prove life-saving during the impending war.
But in one of medicine’s uglier ironies, Dr. Drew was ineligible to donate blood, even after he became manager of Presbyterian Hospital’s blood supply and later, managed America’s Blood for Britain program. The racial obstacles he faced led him to carve out another legacy for himself – a racial one – and as the first African-American to become a member of the American Board of Surgery, he became outspoken about the racial practices common in medicine at the time.
The oldest son of a carpet layer and a teacher, Charles Drew grew up in Washington D.C. His athletic talents won him a scholarship at Amherst College, where he graduated in 1926. He dreamed of becoming a doctor and worked as a coach and biology instructor at Morgan University in Baltimore to raise money for medical school after finishing college.
But there was a problem: only two medical schools in the United States accepted African-American students. Howard University rejected him, and Harvard deferred him for a year, so he took his dream of becoming a physician to Montreal’s McGill University, where he graduated in 1933, second in his class, with a Doctor of Medicine and a Master of Surgery.
Drew stayed in Canada for his internship and residency at McGill’s Royal Victoria Hospital and Montreal General Hospital, examining issues related to blood transfusions. He returned to the US in 1935 as an instructor at Howard University’s College of Medicine before receiving a Rockefeller Fellowship at Columbia University in 1938.
It was during his time at Columbia that Drew developed his pioneering method to isolate and preserve blood plasma by separating it from the other blood components, allowing scientists to stabilize and freeze it for up to two months. This was a seismic breakthrough in hematology; at the time, there was no refined method to separate blood into components and whole blood’s shelf life was only one week. This revelation became the basis of the doctorate thesis he wrote in 1939 while Europe was sliding into war and America was two years away from joining it. In other words, it was just in time.

(

Drew’s innovation was put to use in 1940 as World War II rampaged through Europe. In combat situations, plasma is used as transfusion support to treat shock and replace lost fluids, and Drew’s expertise made him the perfect leader of Blood for Britain, the world’s first large-scale blood drive and a relief effort run by the American Red Cross to collect plasma in the US and ship it to Britain to aid injured British soldiers.
This program not only provided immediate relief and over 5,000 liters of plasma saline solution to the UK, but also served as a model for what might become necessary if and when the US entered the war. It also introduced mobile blood collections and America’s first bloodmobiles.

However, Dr. Drew became discouraged with the racial prejudice he saw in these war efforts. At first, the military excluded African American donors, meaning that Drew himself couldn’t donate to his own Blood for Britain initiative. He left the Red Cross in 1941 to become the Chair of Surgery at Howard University, but in 1942, after it was decided that African-Americans could indeed donate blood but that it would be kept separate from that of white donors, Drew had this to say:
“I feel that the recent ruling of the United States Army and Navy regarding the refusal of colored blood donors is an indefensible one from any point of view. As you know, there is no scientific basis for the separation of the bloods of different races except on the basis of the individual blood types or groups.”
Drew spent the rest of his career as a professor at Howard and the chief of surgery at its Freedmen’s Hospital, training and mentoring African-American surgeons, petitioning medical organizations for equal admission regardless of race, and speaking out against the Red Cross’ discriminatory donation practices. He was awarded the NAACP’s esteemed Spingarn Medal in 1944 for “the highest and noblest achievement in the preceding year or years” for his plasma collection and distribution efforts.
At the age of 45, Dr. Charles Drew succumbed to his injuries following a car accident in 1950, the same year the American Red Cross ended its policy to segregate blood. For more information on Dr. Charles Drew and his contributions to blood banking, our friends at OneBlood and Department of Defense have put together great videos:
Photos courtesy U.S. National Library of Medicine
Tell Us What You Think!